Arthritis Treatment
There are 2 main categories of arthritis – osteoarthritis and rheumatoid (inflammatory) arthritis.
Osteoarthritis (OA) Treatment
Osteoarthritis (OA) is the wear and tear breakdown of the joint – involving the hyaline cartilage (the smooth shiny white surface that covers the end of the bone), the ligaments, capsule, synovial membrane and the bone surface. Any joint can be affected, but the most commonly affected joints are the knees, hips, ankles, shoulders, hands and spinal/neck joints.
In OA the cartilage starts to break down which causes pain, swelling and stiffness in the joint. As the OA progresses the soft tissues around the joint (capsule, synovial membrane and ligaments) thicken and stiffen and also become a source of pain and swelling. The bone surface can also be affected with spur formation (osteophytes), bony stress reaction and bony and cartilage fragments inside the joint.
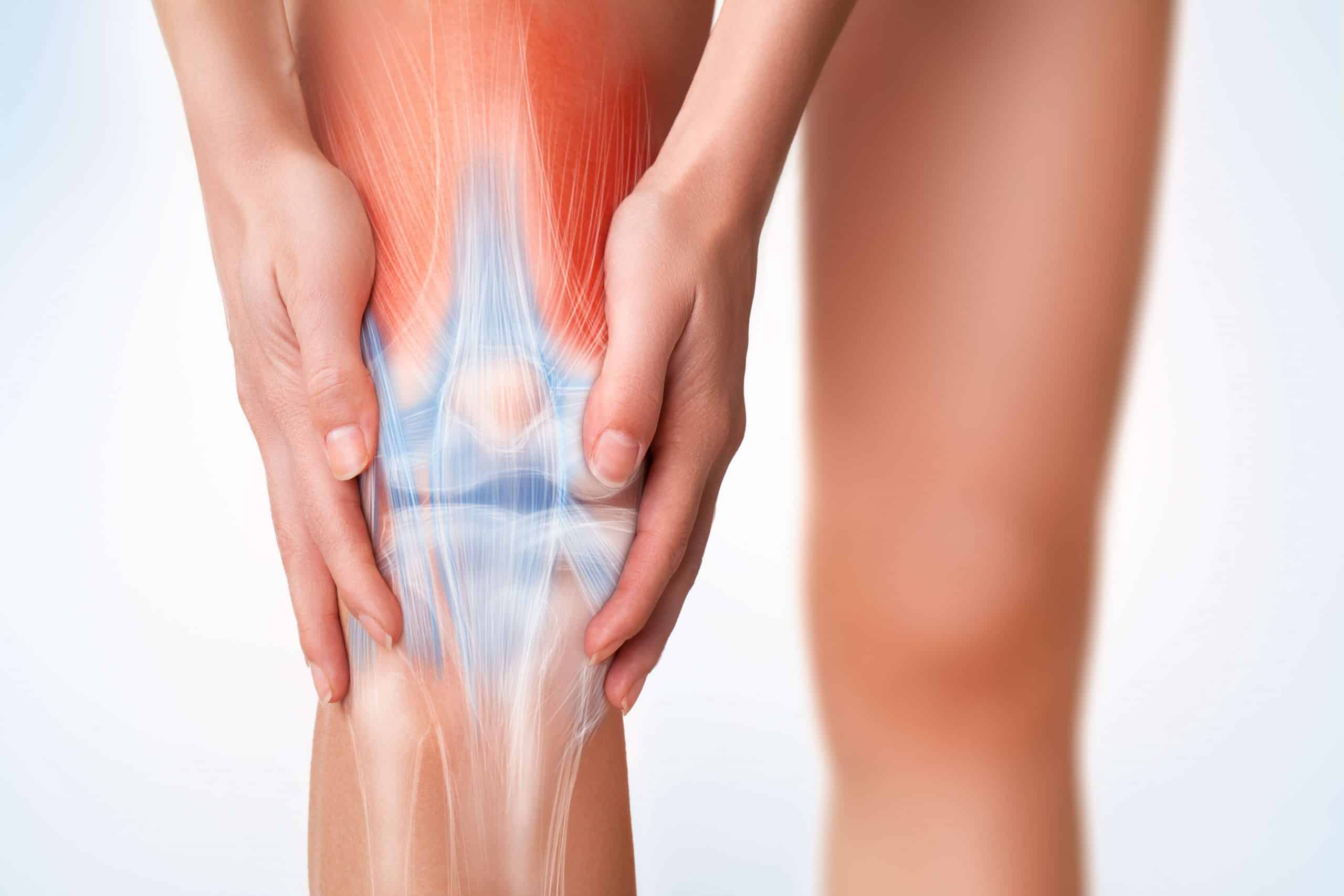
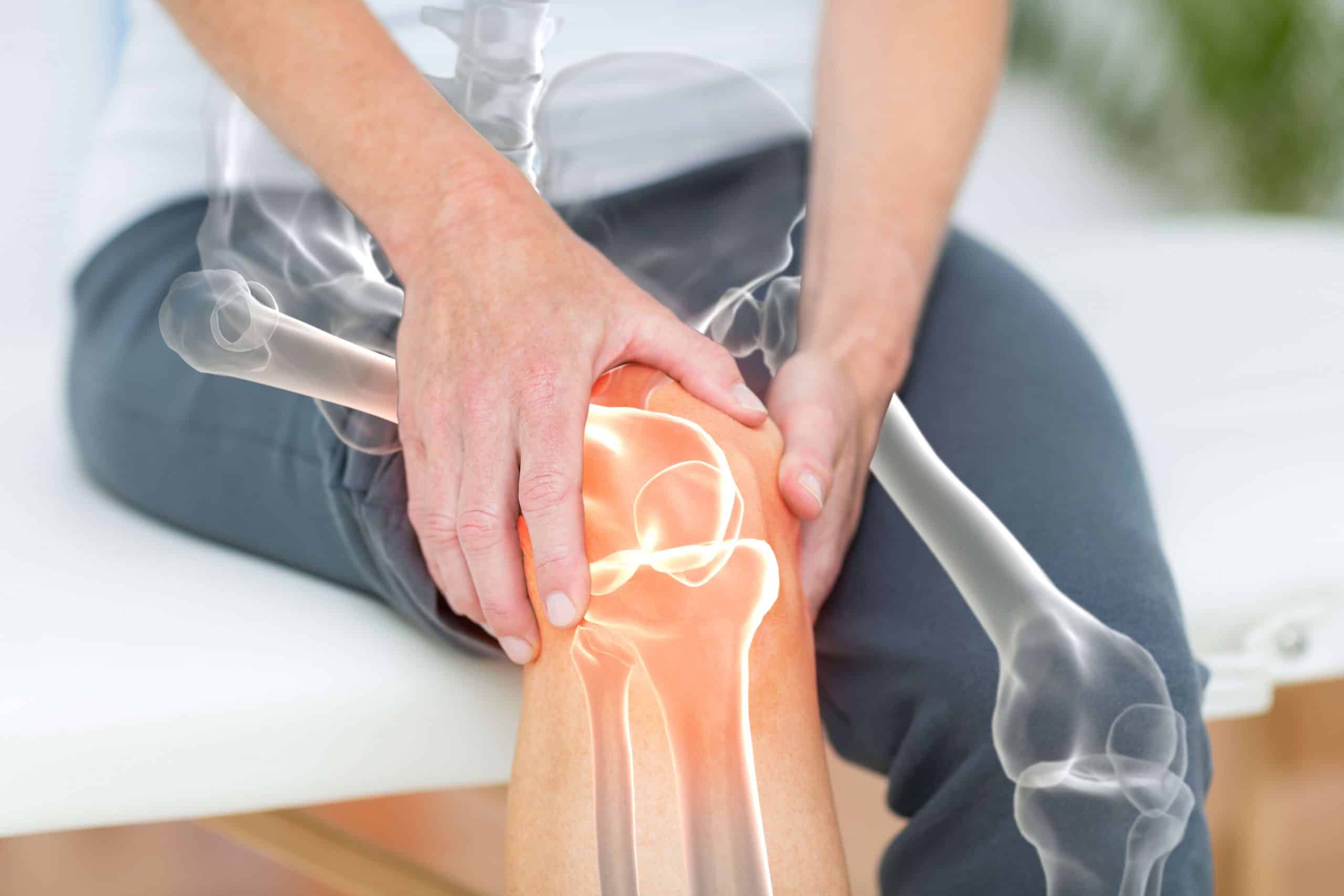
Many people with osteoarthritis decrease or stop exercising at the level suggested by the World Health Organisation (150 minutes per week of moderate-vigorous exercise) due to fear of making their arthritis worse. However, a recent medical research trial studied 1978 knees with OA or at a high risk of OA participating in different levels of physical activity over 4 years. They found no increased progression on OA shown on the Xrays in the exercising people compared with the sedentary people over a 4 year period.
This research proves that people who have knee OA or are at risk of knee OA (meaning they have 2 or more risk factors such as obesity) will not make their arthritis worse by exercising at the recommended intensity for 30 minutes 5 days per week. This is fantastic news for people who have risk factors for OA or have OA as well as other health issues that would benefit from exercise.
The best way of managing and treating osteoarthritis is to maintain movement of the joints, increase the strength in the muscles around the knee and decrease body weight (if applicable). Let our team build you a treatment plan today.
Rheumatoid Arthritis (RA) Treatment
Rheumatoid Arthritis (RA) is an autoimmune inflammatory disease that has a systemic effect on the entire body, not just the joints. The disease affects primarily the synovial membrane around the joints, but can also affect the surrounding soft tissue structures, then causes the erosion of the underlying cartilage and bone. Long term this results in pain, swelling, loss of function and joint deformity.
RA is diagnosed by a Rheumatologist and managed by a team consisting of your specialist, GP, physio and OT. From a physiotherapy perspective, management is aimed at improving/maintain joint movement and function, decreasing and managing pain, improving the muscular strength around the affected joint, minimising contributing factors and improving quality of life.

Our Services
Your GP and Rheumatologist specialist will provide appropriate assessments and medications. Physiotherapy can then be effective as part of your management team in the following areas:

Physiotherapy

Education, pacing, mindfulness and activity guidelines
Exercise prescription